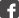DENTAL ABSCESS
ARTICLE PUBLISHED IN THE MAGAZINE “30 DAYS OF HEALTH”, ISSUE Νο105, JULY 2015
What is a dental abscess?
As abscess is defined the localized collection of pus within the tissues. It is due to pyogenic microorganisms, such as streptococci and staphylococci. The abscess cavity contains abundantly neutrophils, polymorphonuclears, necrotic tissues, microbial colonies, lymphocytes and other defensive cells.
Types of abscesses
Odontogenic-dentoalveolar abscess
The dentoalveolar or otherwise periapical abscess is the localized purulent, exudative collection in the apex of the affected tooth.
Microbes of the oral environment penetrate in the tooth, due to dental caries, botched prosthetic work or filling, infecting it and the tooth becomes necrotic. The bacteria and the necrotic toxins reach the bone marrow cavities through the system of root canals. The “response” of the immune mechanism to the bacterial infection is the purulent inflammation. Intense osteoclastic activity is observed, which results to the attenuation of the bone substrate. Subsequently, the pus infiltrates the adjacent soft cells and causes either intraoral or extraoral swelling.
The abscess goes through various phases until it “matures”. Initially it is moderately hard, and subsequently its composition becomes elastic-fluctuant and eventually, following the paths of least resistance through the adjacent tissues it is drained through the pore of the fistula.
The dentoalveolar abscess is distinguished in acute and chronic. Acute abscesses are characterized by acute, persistent, constant, unbearable pain. On the contrary, a chronic abscess can be manifested as a mild pain, with periodicity and a feeling of pressure in the area of the affected tooth. However, most of the times it is totally asymptomatic and is discovered in an random X-ray check as a well circumscribed radiolucent area with undefined limits in the root of the affected tooth. The acute abscess can be transformed into chronic abscess.
What is the clinic picture of the dental abscess?
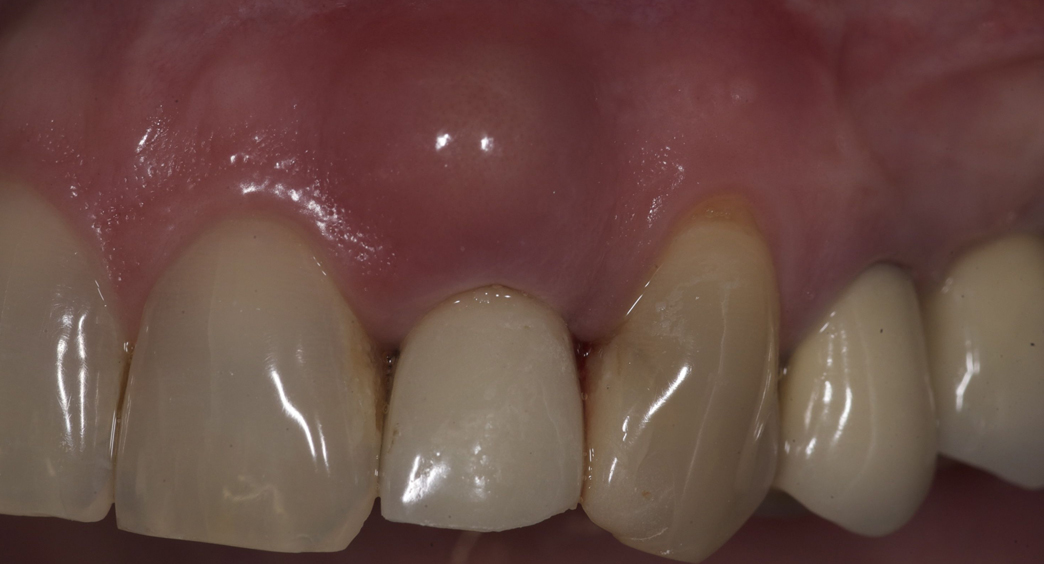
Depending on the position of the tooth in the dentition and the expansion of the abscess, the swelling can be observed in various locations. It is usually discovered through an inflation in the gingivomandibular or the gingivolabial sulcus and less often in the palate, or through a fistula (a “pimple” as it is described by many patients). If the abscess has spread to adjacent tissues, then a swelling is observed in the area of the lips, the cheek, the submental or submandibular space. The skin can be warm at touch and be characterized by a redness.
In some cases, which can be correlated with a bad health history, in an extensive spread of the purulent fluid, associated symptoms can be also observed, such as fever, malaise and ipsilateral lymphadenitis.
How is the diagnosis of a dental abscess made?
It is particularly important that the treating dentist discovers the tooth that is responsible for the abscess by evaluating both the radiographic and the clinical findings. The “treatment” of wrong teeth is not a rare case, because the abscess, is not always located in the radiographically characteristic position at the top part of the apex in a perfect perimeter. Sometimes it is located between two teeth, as the result of the exit of microbes through some lateral root canal or the abscess can include the adjacent teeth due of its tendency to expand. Teeth with dental caries close to the pulp pocket, crowns with decayed edges, incomplete root canal treatments that have been made before, teeth with intense percussion are implicated, compared to other adjacent teeth.
How is the dental abscess treated?
The primary objective is to provide immediate relief. Through a hole in the chewing surface of the tooth, the dentist shall try to drain the purulent fluid. If it is possible, the dentist will proceed to the intraoral breaking of the abscess or to the curettage of the fistula. In a second phase, the root canal treatment shall take place. It must be pointed out how important is to find the tooth that is responsible for the abscess, as well as to perform a proper treatment, with a complete cleaning of the entire labyrintine root canal system of its microbial content. This is achieved with the use of special medicines. It is recommended to the patient to take antibiotics and painkillers as a complementary therapy. It is remarked that the action of antibiotics and anti-inflammatory drugs is totally complementary. They are administered only for the faster control of the symptoms. Due to the necrosis of the tooth and the degeneration of blood vessels, the antibiotics cannot reach the tooth bacteria, which are solely responsible for the development of the abscess. Paracetamol, due to the inflammatory character of the entire process, can offer relief only in large doses. Finally, frequent mouth washes with lukewarm chamomile tea are quite helpful, as the pressure of the abscess cavity is relieved. The pressure in the nerve branches is responsible for the unbearable pain that is caused.
Periodontal-gingival abscess
The cause of the periodontal disease is microbial. The formation of pockets (areas where the connection between the teeth and the gum tissue is lost) is an inflammatory process. The pockets are full of microbes and periodontal pathogenic bacteria. When they are blocked by calculus and due to the fact that food and foreign objects are stuck in them, the inflammation cannot be drained and a pus collection is formed. The gingival abscess can only occur in the gums. If the periodontal abscess is not treated it shall expand periapically with the parallel attenuation of the bone and can infect the tooth through the apex, that is, by following the inverse path of the one of the periapical abscess. For its treatment, curettage is performed as well as the drainage of the abscess, rinsing of the area or application of chlorhexidine gel, while instructions regarding the proper oral hygiene are given.
Pericoronal abscess-pericoronitis
Pericoronal abscess can develop in the operculum of a semi-impacted tooth,
more frequently of the third molar (wisdom tooth) and more usually at the age of 17-24 years, during its eruption. Microbes are accumulated between the tooth and the gums due to the difficult oral hygiene. The covering tissues are inflamed, become edematous and painful. During chewing it is easy that the area is injured, which will lead to the development of more microbial colonies in the interior, leading to a vicious cycle. This is often accompanied by an outflow of pus, malodor and difficulty in swallowing food. The recommended treatment is the removal-excision of the inflamed gingival tissue, the rinsing of the area with chlorhexidine and it is also recommended to the patient to follow a good oral hygiene.
Are there any dangers for the patient’s health?
Before the discovery of penicillin, many patients died due to abscesses of the neck and facial region. The purulent exudate tends to expand in the adjacent tissues through the path of the least resistance. Initially, the infection of the bones of the upper and lower jaw can transform into osteomyelitis. It the muscles are affected there is difficulty opening the mouth. Abscesses in the upper jaw may infect the sinus. If the abscess is not treated promptly and properly, it can spread from the oral cavity to the ground of the mouth, the neck and the upper respiratory tract, blocking the airways (Ludwig’s angina), a condition which is quite life-threatening, and can subsequently spread in the lower respiratory tract. Other possible complications are endocarditis and cavernous sinus thrombosis. In complicated cases, antibiotics are administered intravenously, supportive treatment is applied, corticosteroids are administered and many surgeons proceed to the extraoral incision-breaking, with the placement of drainage tubes.
Does the tooth need to be extracted?
It is very important that abscesses are promptly and properly treated. Even in an aggressive and very painful for the patient condition, the treating dentist must examine all the parameters for the treatment and the proper future restoration of the patient’s health. The extraction of the tooth does not consist a treatment of choice, if the tooth can be preserved in healthy conditions with the adjacent tissues. The preservation of teeth, even in extreme inflammatory conditions, is feasible. It is therefore, the duty of the dentist, who will have to be calm and highly trained, as the Dentist-Endodontist, to assure the patient that these acute symptoms will be very soon eliminated. For this reason, the specialists will have to be well informed about modern methods of treatment and restoration of their oral health. The very rapid development of medical specialties, as well as the proper updating of dentists, consists a guarantee for the proper care of patients.
Constantinos Laghios, Dental Surgeon-Endodontist, M.S., Aikaterini Georgaki, Dental Surgeon